When someone says they have inflammatory bowel disease, it doesn’t tell the whole story. Two very different conditions fall under that label: Crohn’s disease and ulcerative colitis. They share symptoms like belly pain, diarrhea, and fatigue-but how they behave in the body, where they strike, and how they’re treated couldn’t be more different. Knowing which one you’re dealing with changes everything-from what tests you need to whether surgery could actually cure you.
Where the Inflammation Happens
- Ulcerative colitis only affects the colon and rectum. It starts at the very end of your large intestine and moves upward in a continuous line. If you have it, every inch of inflamed tissue connects to the next. There are no gaps. It never touches your small intestine, stomach, or mouth.
- Crohn’s disease can show up anywhere along the digestive tract, from your mouth to your anus. Most often, it hits the end of the small intestine (ileum) and the beginning of the colon. But it can skip around. You might have patches of healthy tissue between inflamed areas-what doctors call "skip lesions." That’s not just a detail; it’s a key clue in telling the two apart.
This difference in location matters because it affects what symptoms you feel. People with ulcerative colitis usually feel urgency to go to the bathroom and notice blood in their stool. Crohn’s patients often report pain around the navel or lower right abdomen, and some struggle with malnutrition because the small intestine isn’t absorbing nutrients properly.
How Deep the Damage Goes
The colon has layers. Think of it like an onion. Ulcerative colitis only eats away at the top layer-the mucosa, the lining that touches food and stool. That’s why bleeding is so common. It’s just the surface breaking down.
Crohn’s disease goes deeper. It punches through all layers: mucosa, submucosa, muscle, even the outer covering. This transmural inflammation is why Crohn’s leads to complications like strictures (narrowing from scar tissue) and fistulas (abnormal tunnels connecting organs). A fistula might link your intestine to your bladder, skin, or another part of your gut. These happen in about 25% of Crohn’s patients over time. In ulcerative colitis? Less than 5%.
What Tests Reveal
There’s no single blood test that says "Crohn’s" or "ulcerative colitis." Diagnosis comes from putting together clues.
A colonoscopy is the gold standard. In ulcerative colitis, doctors see a smooth, red, inflamed lining from the rectum up. Pseudopolyps-small bumps of healing tissue-often appear. In Crohn’s, they see patchy inflammation, cracked skin like cobblestones, and sometimes deep ulcers.
Imaging helps too. An MRI enterography can spot fistulas and thickened bowel walls, common in Crohn’s. Capsule endoscopy (a pill-sized camera you swallow) finds small bowel damage in about 70% of Crohn’s cases that a colonoscopy misses.
Blood and stool markers add more pieces. Fecal calprotectin (a protein released during gut inflammation) is elevated in both, but higher in ulcerative colitis on average. The pANCA antibody test is positive in 60-70% of ulcerative colitis patients but only 10-15% of Crohn’s patients. It’s not perfect, but it’s a strong hint.
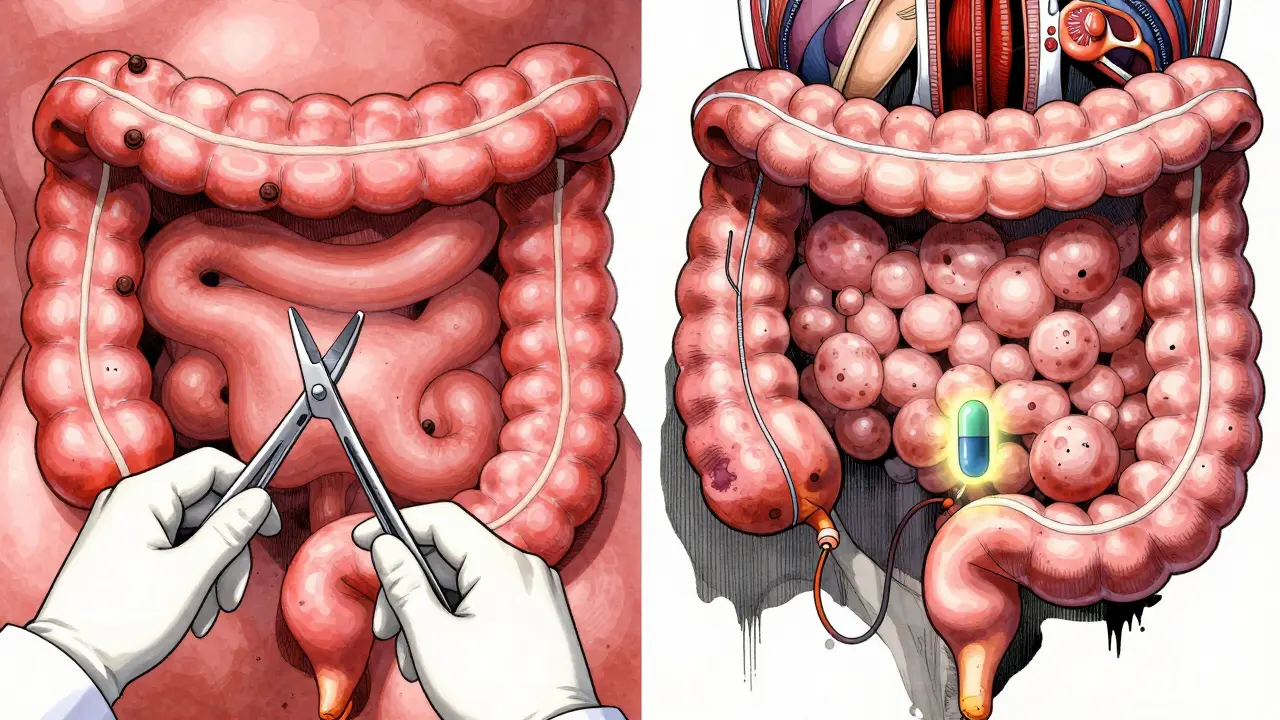
Complications That Set Them Apart
Both conditions raise your risk of colon cancer if inflammation lasts more than 8-10 years. But beyond that, their dangers diverge.
- Crohn’s risks: strictures (33% lifetime risk), fistulas (25%), abscesses, and malnutrition from poor nutrient absorption. About half of people with Crohn’s will need surgery at least once, but it doesn’t cure the disease-new inflammation often returns near the surgery site.
- Ulcerative colitis risks: toxic megacolon (a rare but life-threatening swelling of the colon, affecting 5% during severe flares) and primary sclerosing cholangitis (a liver disease affecting 3-7% of UC patients, but less than 1% of Crohn’s patients).
Extraintestinal issues-problems outside the gut-affect both. Joint pain, skin rashes like erythema nodosum, and eye inflammation show up in about 25-40% of IBD patients regardless of type. But if you have liver or bile duct trouble, it’s far more likely to be linked to ulcerative colitis.
Treatment Differences
Both can be treated with anti-inflammatories, immunosuppressants, and biologics-but how they’re used changes based on where the disease lives.
For ulcerative colitis, topical treatments work wonders. Enemas and suppositories deliver 5-ASA drugs (like mesalamine) right to the inflamed colon. In mild to moderate cases, this puts patients into remission 60-80% of the time.
Crohn’s disease usually needs systemic treatment-drugs that travel through the whole body. That’s because the inflammation isn’t just in the colon. Medications like azathioprine or biologics (infliximab, adalimumab) are often used early. The SONIC trial showed azathioprine helped 40-50% of Crohn’s patients reach remission in under 17 weeks.
Biologics help both, but they work better in Crohn’s. At 54 weeks, about 30-40% of Crohn’s patients on anti-TNF drugs like infliximab go into remission. For ulcerative colitis, that number is 20-30%.
Surgery: Cure vs. Management
This is one of the biggest differences.
If you have ulcerative colitis and your symptoms don’t respond to medication, removing the entire colon and rectum (a total proctocolectomy) can cure you. Surgeons can then create an internal pouch from the small intestine to replace the rectum. About 10-15% of UC patients end up having this surgery within 10 years.
Crohn’s disease doesn’t work that way. Even if you remove the damaged part of your intestine, the disease almost always comes back nearby. About half of Crohn’s patients need another surgery within 10 years. Surgery helps relieve symptoms, but it’s not a cure.
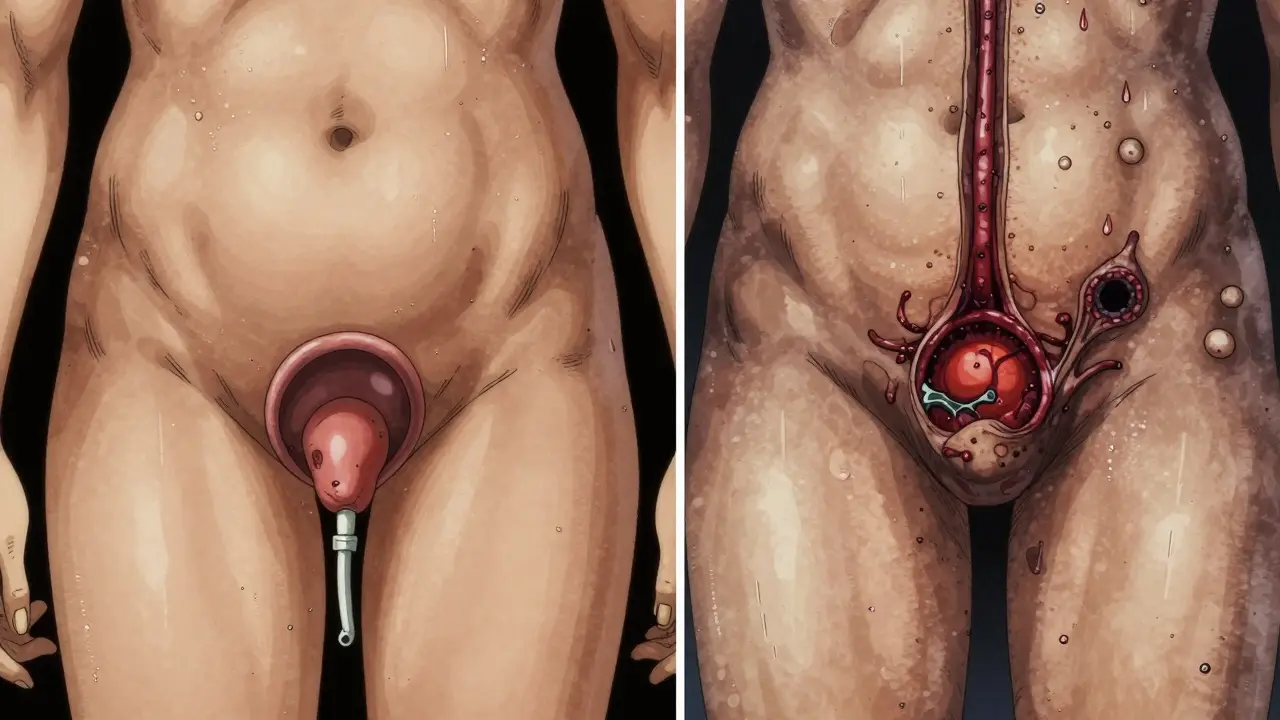
What Patients Say
Real-world experiences back up the medical data. In patient forums, people with ulcerative colitis talk about sudden urges to go and rectal bleeding as their biggest daily struggles. Crohn’s patients are more likely to say they’re worried about weight loss, nutrient deficiencies, or pain after eating certain foods.
On Reddit’s r/IBD community, stress is the top flare trigger for ulcerative colitis (cited in 62% of posts). For Crohn’s, it’s food-dairy, high-fiber items, or greasy meals. That doesn’t mean food causes the disease, but it can make symptoms worse, especially when the small intestine is involved.
What If You Don’t Know Which One You Have?
It happens. About 10-15% of people with IBD are initially diagnosed with "indeterminate colitis." Their symptoms and test results don’t clearly point to Crohn’s or ulcerative colitis. This doesn’t mean something’s wrong-it just means the disease hasn’t revealed its full pattern yet.
Follow-up over time helps. If someone initially thought to have ulcerative colitis later develops fistulas or small bowel involvement, they’re likely reclassified as Crohn’s. A Swiss study found that 12.3% of people diagnosed with UC were later found to have Crohn’s after five years.
Doctors now focus less on where the disease starts and more on how it behaves. Is it just inflamed? Or is it causing strictures or fistulas? The behavior tells you more about future risks than location alone.
The Bigger Picture
IBD affects about 3 million Americans, with nearly equal numbers of Crohn’s and ulcerative colitis cases. Rates are rising globally, especially in countries undergoing rapid urbanization. In Australia, estimates suggest 1 in 250 people live with IBD-similar to the U.S. and Europe.
Costs are high. The average yearly medical cost for severe Crohn’s is over $38,000. For severe ulcerative colitis, it’s nearly $38,500. That’s because both need frequent monitoring, hospital visits, and expensive biologics.
New treatments are on the horizon. Fecal microbiota transplants (FMT) have shown 32% remission rates in ulcerative colitis in recent trials. For Crohn’s, the same approach only helped 22%. Drugs like mirikizumab (for Crohn’s) and etrolizumab (for UC) are in late-stage trials and could be approved by late 2024.
What’s clear is this: Crohn’s disease and ulcerative colitis aren’t the same illness with different names. They’re distinct diseases with overlapping symptoms but very different rules. Getting the right diagnosis isn’t just about labels-it’s about choosing the right treatment, planning for the future, and knowing what to expect.
Can you have both Crohn’s disease and ulcerative colitis at the same time?
No, you can’t have both at the same time. They are two separate conditions under the umbrella of inflammatory bowel disease. If someone’s symptoms don’t clearly point to one or the other, they might be labeled as having "indeterminate colitis"-but that’s a temporary classification. Over time, as the disease progresses, it almost always becomes clear which one it is. Most people with indeterminate colitis are later reclassified as either Crohn’s or ulcerative colitis.
Does diet cause inflammatory bowel disease?
No, diet does not cause Crohn’s disease or ulcerative colitis. These are autoimmune conditions triggered by a mix of genetics, immune system misfires, and environmental factors like antibiotics, smoking, or early-life gut infections. But food can definitely make symptoms worse. High-fat meals, dairy, or fiber-rich foods may trigger bloating or diarrhea in some people, especially if their intestine is already inflamed. That’s why diet plans are often personalized-not to cure the disease, but to help manage daily symptoms.
Is IBD the same as IBS?
No, they’re completely different. IBD (Crohn’s and ulcerative colitis) involves chronic inflammation, tissue damage, and higher risks of complications like cancer or surgery. IBS (Irritable Bowel Syndrome) is a functional disorder-meaning the gut looks normal on scans and biopsies, but it doesn’t work right. IBS causes cramping, bloating, and changes in bowel habits, but it doesn’t cause bleeding, weight loss, or structural damage. The treatments are totally different too.
Can you outgrow inflammatory bowel disease?
No, IBD is a lifelong condition. Even if you’re in long-term remission and feel completely fine, the underlying immune dysfunction is still there. That’s why regular check-ups and monitoring are important-even when you’re not having symptoms. Some people go years without flares, especially with modern treatments, but the disease doesn’t disappear. Stopping medication without medical advice can lead to a return of inflammation.
Does stress cause flare-ups?
Stress doesn’t cause IBD, but it can make flare-ups worse. Studies show that people with ulcerative colitis often report stress as their top trigger. For Crohn’s, food and infections are more commonly cited. That doesn’t mean stress is the enemy-it’s one of many factors. Managing stress through sleep, exercise, or therapy can help reduce how often flares happen and how severe they are. But it’s not a substitute for medical treatment.

tia novialiswati
February 25, 2026 AT 07:43Wow, this breakdown is SO helpful! I’ve had UC for 8 years and honestly, I didn’t realize how much Crohn’s differs in depth and behavior. The part about fistulas and skip lesions? Mind blown. 🙌 Thanks for making it so clear - I’m sharing this with my support group!
Christopher Brown
February 25, 2026 AT 17:33Pathetic. You people treat IBD like a yoga class. It’s a chronic, life-ruining disease. Stop romanticizing it with emojis and feel-good posts. Get real.
Kenzie Goode
February 27, 2026 AT 14:47I’m sitting here crying because this article nailed everything I’ve been trying to explain to my family for years. The difference between UC and Crohn’s isn’t just medical - it’s emotional. I thought I was alone until now. Thank you.
Dominic Punch
March 1, 2026 AT 13:04One thing missing here is the role of microbiome diversity. Recent studies (2023, Gut Journal) show that Crohn’s patients have significantly lower Faecalibacterium prausnitzii levels than UC patients - which may explain why FMT works better for UC. Also, smoking worsens Crohn’s but may protect against UC. Weird, right? Science is wild.
Stephen Archbold
March 2, 2026 AT 14:36Just had my 3rd colonoscopy last week. Docs said I’ve got UC but I swear I’ve got Crohn’s vibes - pain in my right side, weight loss, no rectal bleeding. Guess I’m one of those 12% who got mislabeled. Fingers crossed for the next scan.
Nick Hamby
March 4, 2026 AT 01:06It’s fascinating how the language we use to describe these conditions shapes patient outcomes. When we say "cure" for ulcerative colitis, we offer hope. When we say "management" for Crohn’s, we inadvertently signal inevitability. Language isn’t neutral - it’s therapeutic. This distinction deserves deeper bioethical consideration.
Gabrielle Conroy
March 4, 2026 AT 08:03YES! The fecal calprotectin point? SO IMPORTANT. My doc didn’t even mention it until I brought it up. Also, the fact that UC patients respond better to topical meds? I’ve been using Asacol suppositories and it’s been life-changing. 🙏✨
Spenser Bickett
March 4, 2026 AT 10:40So let me get this straight… you’re telling me I didn’t get this disease because I ate too much pizza? I’m devastated. My therapist says I have trauma around tacos. Guess I’ll be crying into my gluten-free kale smoothie now.
Christopher Wiedenhaupt
March 5, 2026 AT 23:24My brother has crohns. He had surgery last year. They removed his terminal ileum. Now he's on adalimumab. He lost 40lbs. He's still tired all the time. He says he's not cured. He says he's just less sick. This article got it right.
John Smith
March 6, 2026 AT 08:22Wow. So much text. So little substance. You people treat a chronic illness like a Netflix doc. Just take your meds and stop posting.
Shalini Gautam
March 7, 2026 AT 13:40India’s IBD rates are rising fast - urbanization, processed food, antibiotics in childhood. My sister got diagnosed at 22. No family history. This isn’t just a Western problem anymore.
Natanya Green
March 8, 2026 AT 18:13OMG I just realized I’ve been blaming my stress for my flares… but what if it’s actually the dairy? Or the gluten? Or my cat? I’m going to cry. I’m going to scream. I’m going to eat a burrito and pray.